For Therapists & Psychiatrists
We handle everything from claim submission to payment posting so you can spend more time with your patients.
Compliant
Nationwide


Mostly mental health providers lose thousands of dollars every year because of billing errors. A wrong CPT code. A missing modifier. A late prior authorization. These small mistakes lead to denied claims, delayed payments and lost revenue. Mental Health Billing SRG makes sure your claims go out clean, every single time. We verify eligibility, handle prior authorizations, submit accurate claims, and follow up until you get paid. No more chasing insurance companies. No more stacks of unpaid claims. Just clean billing and full reimbursement on time.
We offer complete billing and revenue cycle management services built specifically for mental health providers. From your first patient visit to the final payment.

Wrong codes mean denied claims. Denied claims mean lost revenue. We use accurate CPT, ICD-10 and HCPCS codes for each service, backed by a thorough pre-billing review. From therapy sessions to psychiatric evaluations, we make sure every claim is clean and every reimbursement arrives on time. The result? Fewer denials. Faster payments. And a healthier bottom line for your practice.

Our RCM services keep your cash flow steady and your practice financially healthy. We track every step of the billing cycle, identifying issues early and fixing them fast. Less revenue leakage. More money in your pocket. It is more than just submitting claims. It covers everything from patient registration to final payment collection.

Credentialing is slow, complex and easy to get wrong. One missing document can delay your entire enrollment and cost you months of unbillable services. Our experts manage your full credentialing process of CAQH, PECOS and NPI.

Skipping insurance verification is one of the most expensive billing mistakes a practice can make. Mental Health Billing SRG verifies every patient’s coverage before their visit, checking active insurance, co-pays, deductibles and benefit limits. We flag any issues before they become denials. So your claims go out clean and your payments come in on time.

Prior authorization is one of the most time-consuming parts of mental health billing. Every insurance payer has different requirements. One missed step and your claim gets denied. We handle prior authorization submissions for all major payers. We track approval status, follow up on pending requests and flag expiring authorizations. So treatment never gets delayed because of a paperwork issue.

Every service your providers deliver needs to be entered accurately and on time. Errors at the charge entry stage cause problems down the line, wrong codes, missed charges, delayed claims. Our team reviews and enters all charges with precision. We make sure every service is captured, coded correctly and ready for clean claim submission.

We submit all claims electronically for faster processing. Before every submission, our team runs a thorough review, checking codes, patient information, payer requirements and documentation accuracy. Our clean claim rate is 98%. That means fewer rejections, faster approvals and quicker reimbursements for your practice.

We handle ERA (Electronic Remittance Advice) and EOB (Explanation of Benefits) reconciliation, making sure every payment is posted correctly to the right patient account. Accurate payment posting keeps your books clean and your financial reports reliable.

Our team runs proactive accounts receivable follow-ups on every outstanding claim. We contact payers, track responses and push for resolution fast. We reduce your days in AR so cash keeps flowing into your practice. Unpaid claims don’t just disappear. They sit in your accounts receivable and quietly drain your revenue.

Mental Health Billing SRG handles the entire denial resolution process from root cause analysis to appeal preparation to payer negotiation. We move fast, document everything and fight for every dollar your practice deserves. And we track denial trends so the same mistakes never repeat.

We handle patient billing professionally and respectfully. From co-pay collection to deductible follow-ups and outstanding balance reminders, we make sure your practice gets paid without damaging your patient relationships.

A smooth billing process starts with strong practice management. We integrate directly with your existing EHR and practice management software, no disruption to your workflow. Our team supports all major platforms and makes sure your billing system works seamlessly from the very first day.

Not sure where your revenue is leaking? A billing audit will tell you. We review your entire billing process, claims history, denial trends, coding accuracy and AR health. Our experts identify exactly where money is being lost and give you a clear plan to fix it.
Every patient has a unique treatment plan, different insurance coverage and specific payer requirements. These differences create billing challenges that cost practices thousands of dollars every year.
Even one small coding error can get your claim denied. The average denial rate in mental health billing is between 15% and 20%. Our pre-billing review catches errors before claims go out keeping our clean claim rate at 98%.
Every insurance payer has its own prior authorization rules. Submitting it incorrectly means an instant denial. We manage entire prior authorization process for every payer.
Credentialing can take 90 to 120 days when not handled correctly. Our credentialing specialists prepare and submit every application accurately. We follow up regularly with payers to speed up the process and avoid costly holdups.
Incomplete session notes, missing diagnoses and unclear treatment plans are all common triggers. We review your documentation against payer requirements before every claim is submitted. This keeps your practice safe from compliance audits.
Uncollected patient payments are sources of silent revenue loss. We handle patient collections professionally, sending clear statements and following up on outstanding balances. Your practice gets paid what it has earned without damaging patient relationships.
Specialized billing expertise across all mental health specialties

Slow payments and unpaid claims are two of the biggest financial problems mental health practices face. Our billing specialists take full control of your revenue cycle. We handle everything from accurate claim submission to automatic follow-up on every pending claim. No manual chasing. No missed payments. Just steady, reliable cash flow.
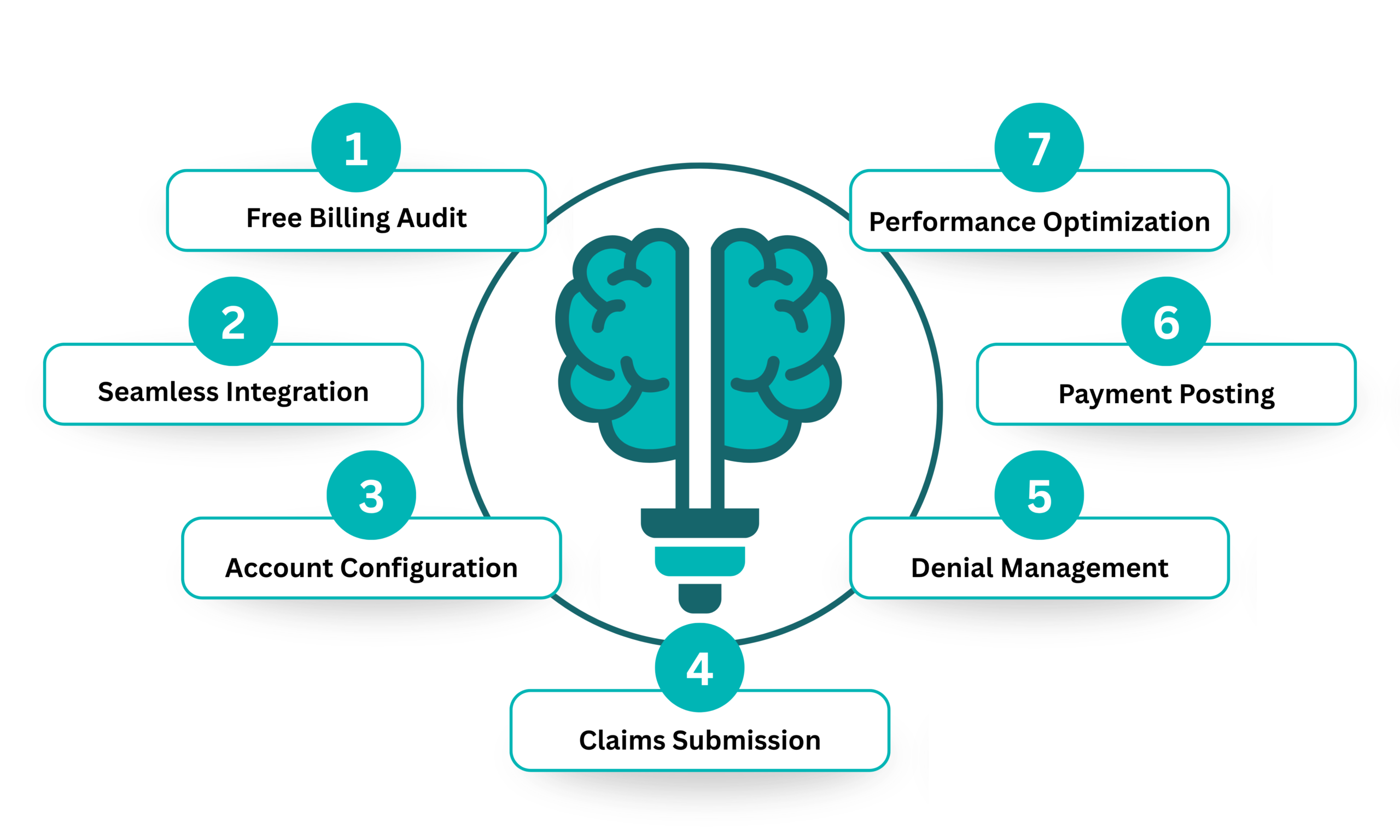
Mental Health Billing SRG has built a proven process that makes the transition smooth, fast and stress-free. From your very first conversation to your first payment posted, every step is handled with precision and care.
We work exclusively with mental health providers. We know your codes, your payers, your challenges, and your compliance requirements inside and out. Here is what makes us the right choice for your practice:

Our entire operation is built around mastering mental health billing. From behavioral health CPT codes to payer-specific policies to compliance requirements, we handle it all with zero learning curve.

Our first-pass claim acceptance rate is 98%, one of the highest in the mental health billing industry. That means fewer denials and faster payments landing in your account.

You will never be passed around a call center or wait days for a response. Every practice gets one dedicated account manager. One point of contact. Always available. Always accountable.

Our billing team holds elite certifications from AAPC and AHIMA, plus specialized training in mental health and behavioral health coding.

Compliance is built into every step of our process. We follow HIPAA privacy and security regulations at all times, keeping your practice audit-ready and fully compliant 365 days a year.

Mental health providers who partner with us see an average revenue increase of 40%+, a reduction in AR days by up to 30% and denial rates that drop below 5%.
Mental Health Billing SRG works exclusively with mental health providers across all 50 states of America, including psychiatrists, psychologists, therapists (LCSW, LMFT, LPC), social workers, counseling centers, addiction treatment centers, ABA therapists and group practices. From E&M coding and telehealth claims to substance use disorder billing, prior authorization management and applied behavior analysis coding we handle every specialty with accuracy.

Getting started with us is simple. No complicated setup. No long waiting periods. Just a clear, proven process that gets your billing running smoothly.

01
We review your current billing process, identify revenue leaks, and show you exactly where money is being lost.

02
We integrate directly with your existing practice management system and EHR with zero disruption to your daily workflow.

03
From charge entry to claim submission to payment posting, we handle every billing task so you can focus entirely on your patients.

04
Every month you will get a detailed performance report, clean claim rate, denial trends, AR health and collections with a clear plan to keep improving your revenue.
Starting a mental health practice is exciting, but poor billing setup can cost you thousands in your very first year. Mental Health Billing SRG offers complete billing and credentialing packages built specifically for new and independent providers, whether you are a solo psychotherapist, an LMHC or a small growing group.
We handle everything from day one, CAQH profile setup, NPI registration, Medicare and Medicaid enrollment, commercial insurance credentialing and full EHR billing system setup. So your revenue cycle runs smoothly from your very first patient visit. Transparent pricing, no hidden fees, just straightforward billing support that grows with your practice.
Mental health service providers have seen an average 48-Hour TAT on claim.
Mental health practices with SRG achieve a clean claim rate of 98%.
Automated patient collections have increased by 40%.
Mental health practices with SRG achieve a 97% net collection rate.
Average denial rates for mental health practices drop to just 5%
20 Accounts Receivable/AR days for mental health providers working with us.
America’s Trusted Mental Health Billing Partner, Serving Providers in All 50 States.

Dr. Sarah Martinez

Dr. James Chen
“The team’s expertise in mental health billing is unmatched. They handle everything from credentialing to denials, and their claim acceptance rate is phenomenal. Highly recommend!”

Rebecca Thompson
“As a group practice with 12 therapists, we needed a billing partner who could scale with us. They’ve been amazing – transparent, efficient, and always available to answer questions.”
Collected for Clients
States Served
We have expertise, tools and dedication to get you paid faster and more consistently. Contact us for more Information. We are ready to help with your billing and coding needs.
We start with a free billing audit to find where your current process is losing money. Then we take over your entire billing cycle, charge entry, claim submission, denial management, payment posting and AR follow-up. Our pre-billing review process catches coding errors before claims go out, which keeps your denial rate low and your cash flow steady.
We support a wide range of mental health providers including psychiatrists, psychologists, licensed therapists (LCSW, LMFT, LPC), social workers, counseling centers, addiction treatment centers, ABA therapists and group practices. We have an experienced team and tools to handle your billing accurately and efficiently.
Patient data security is a top priority at Mental Health Billing SRG. Every part of our billing process is fully HIPAA-compliant. We use secure, encrypted systems for all data storage and transmission. Our team follows strict data handling protocols. Your patients’ information is always protected.
Mental Health Billing SRG specializes in Medicare and Medicaid billing for mental health providers. Our experts understand specific documentation requirements, coverage rules and billing guidelines for both programs to make sure your claims are submitted correctly and reimbursed on time.
Mental Health Billing SRG focuses exclusively on mental health billing. We offer dedicated account managers, transparent pricing starting at 4%, a 98% clean claim rate and full RCM services tailored to needs of private practice therapists and psychiatrists.
Outsourcing your mental health billing saves time, reduces costs and increases revenue. You eliminate the expense of hiring and training in-house billing staff. You get access to specialized billing expertise that reduces denials and speeds up reimbursements. And you get better financial visibility through regular reporting and analytics.
Look for a billing company that specializes in mental health, not one that does general medical billing on the side. Ask about their clean claim rate, denial management process and average days in AR. Make sure they offer dedicated account managers and transparent pricing. Check that they are HIPAA-compliant and experienced with your specific payer mix. Mental Health Billing SRG meets all of these criteria and we back it up with a free billing audit before you commit to anything.
Most behavioral health billing services charge between 4% and 10% of monthly collections. The exact rate depends on your practice size, claim volume and services included. Our pricing starts at just 4%, with no setup fees, no hidden charges.